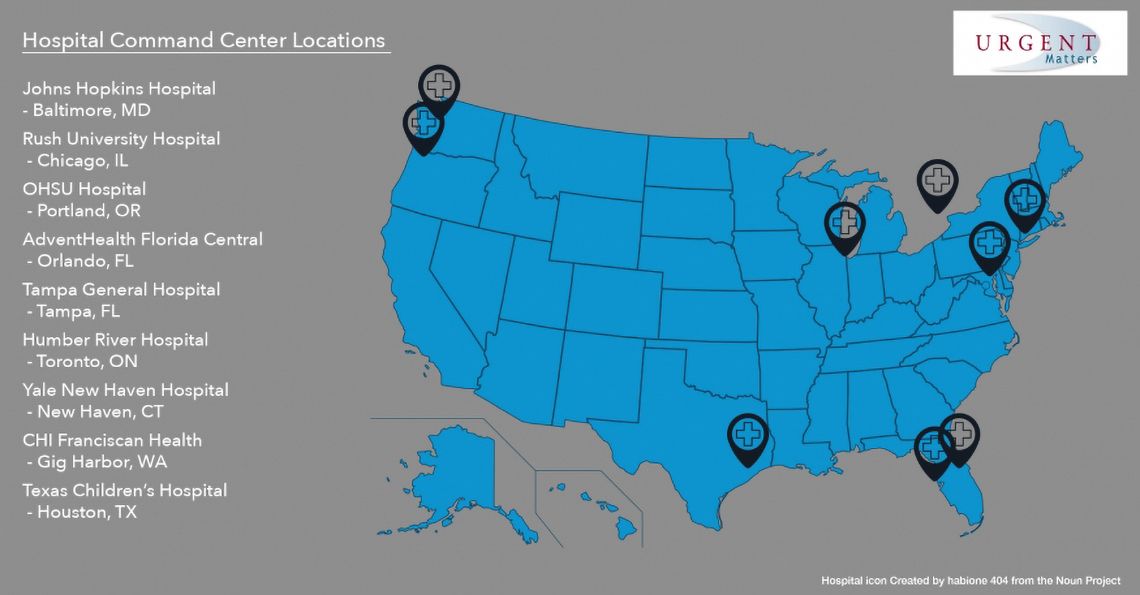
Just like NASA’s mission control analyzes data and provides feedback to optimize a mission in space, a hospital command center does the same for the nurses and clinicians caring for patients on the wards.1 In the past, “incident command centers” were established to temporarily assist health systems to manage operations when confronted with emergencies of a grand scale such as natural disaster. In recent years, command centers have been established as a permanent operational model to manage the complex daily processes of a health system.
Command centers are becoming increasingly common in health systems, often building on an historic, small-scale “bed command” or “bed control” center. These larger, more sophisticated command centers emphasize real-time analytics and co-location of interdisciplinary teams.2 While each was designed for a unique purpose, several common goals emerge. First, command centers aim to improve patient outcomes through centralized quality control and coordination of care. Second, command centers focus on hospital-level flow and efficiency, such as maximizing bed capacity or reducing boarding times. Third, command centers seek to improve coordination between facilities by orchestrating transfers and facilitating communication between partner hospitals.
The command center at Humber River Hospital in Toronto, Ontario is designed to improve patient outcomes by focusing on early detection and prevention of harm for patients at risk of clinical deterioration and sepsis. The command center tracks patients’ risk using the evidence-based National Early Warning Score 2 (NEWS2) algorithm.3 NEWS2 scores are integrated across the hospital’s electronic platforms, allowing for rapid reporting of patients’ risk status.
Other command centers are more focused on increasing hospital efficiency and reducing patient waits, such as ED boarding. The command center at Johns Hopkins Hospital in Baltimore, Maryland has demonstrated a positive effect across several different process measures. For instance, the critical care transport team was dispatched 63 minutes earlier to retrieve patients from outside hospitals. In addition, transfer delays from the operating room were reduced by 70%, and patients in the ED were assigned to beds 30% faster.4 Likewise, the command center in the Yale New Haven Health System in New Haven, Connecticut expanded effective capacity by 148 beds during one of the peak weeks of flu season as compared to the same week in the previous year.5
Finally, Florida Hospital, which typically operates at near-maximum capacity, designed its hospital command center primarily to coordinate care across multiple facilities. Specifically, the hospital system sought to improve patient transfers and communication between sister facilities, as lapses in inter-facility coordination were the source of many logistical problems. Today, the command center coordinates patient care for nine hospitals which treat over two million patient visits and 640,000 ED encounters annually.6
Existing centers have shown improvement in clinical outcomes and clinical workflow, but there is potential for new technologies to build on these initial advancements. With the increasing emphasis on patient-generated data, command centers may soon be able to interface with wearable technologies and home devices to continue monitoring patients after discharge. For now, early evidence supports the use of hospital command centers to enhance the delivery of hospital care.
Sources:
- Kane, Erin M., et al. "Use of systems engineering to design a hospital command center." Jt Comm J Qual Patient Saf. 2019 May;45(5):370-379.
- Ground Control to Major Growth in Hospital Command Centers. (2019, September 10). Retrieved March 19, 2020, from https://www.gehealthcare.com/article/ground-control-to-major-growth-in-hospital-command-centers
- Humber River Hospital. (2019, July 23). Humber River Hospital's Command Centre Generation 2. Retrieved March 30, 2020, from https://www.hrh.ca/2019/07/23/humber-river-hospitals-command-centre-generation-2/
- The Johns Hopkins Hospital Launches Capacity Command Center to Enhance Hospital Operations - 10/26/2016. (2016, October 26). Retrieved March 30, 2020, from https://www.hopkinsmedicine.org/news/media/releases/the_johns_hopkins_hospital_launches_capacity_command_center_to_enhance_hospital_operations
- Confronting the Hospital Capacity Puzzle with Real-Time Dashboards. (2018, June 11). Retrieved March 19, 2020, from https://www.epic.com/epic/post/confronting-hospital-capacity-puzzle-real-time-dashboards
- HealthLeaders. (n.d.). Move Over Star Wars; Hospital Command Centers Take the Spotlight. Retrieved March 19, 2020, from https://www.healthleadersmedia.com/innovation/move-over-star-wars-hospital-command-centers-take-spotlight

Bridget Marcinkowski is a second-year medical student at the George Washington University School of Medicine & Health Sciences. She received bachelor’s degrees in Biology and Nanoscience from Virginia Tech where she also served as an EMT on the Blacksburg Volunteer Rescue Squad. She previously conducted research as a post-baccalaureate fellow at the National Cancer Institute. Her research interests include social emergency medicine, trauma and violence prevention, and health policy.